|
While several quantitative pupillometer devices have been developed, these are still used primarily in research settings, either because the first devices were relatively cumbersome or because they were simply ill-suited to the clinical care environment. Infrared pupillometry is a notable exception because this provides an objective measurement of the PLR. As shown recently, these discrepancies can be as high as 40 %. Moreover, ambient light conditions can impact the validity of visual assessments of the pupil, and exacerbate inter-observer disagreement. The potential therefore exists to compound inaccuracies and inconsistencies, especially given substantial inter-examiner variability. These subjective terms are often applied in the absence of any standardized clinical protocol or definition. Common terminologies employed in the clinical literature to describe the pupillary light reflex (PLR) and pupil size include the following: unilateral, bilateral-nonreactive, fixed, dilated, brisk, sluggish, and nonreactive. 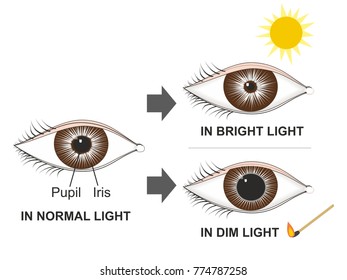 
Pupillary evaluation in the clinical setting is often performed in a subjective manner, with a penlight for reactivity and a pupil gauge for pupil size. The association of these abnormalities with posterior frontal and temporal lesions would suggest that other changes in pupillary function might also be detected, even when the ICP is normal, particularly for lesions adjacent to the brainstem. described changes in pupil shape in a number of patients with an ICP lower than 20 mmHg. In a detailed study correlating changes in pupil shape and intracranial pressure (ICP), Marshall et al. Given their indispensible role in establishing the severity of injury and/or illness, it is not surprising that there is considerable interest in how these parameters may be measured accurately. Measurements of pupil size and reactivity are considered to be of great prognostic importance for patients with critical conditions. The clinical implications for detection of any abnormality have been firmly established in terms of neurological outcome, morbidity, and mortality. Automated quantitative pupillometry is a more reliable method with which to collect pupillary measurements at the bedside.Įvaluation of pupil size and its light reflex mechanism is an integral part of the protocol for the treatment and management of severely brain-injured patients in ICUs worldwide. Standard practice in pupillary monitoring yields inaccurate data. For measurements with small pupils (diameters <2 mm) the error rate was 39 % (24/61). A global rate of discordance of 18 % (72/406) was found between the two techniques when assessing the pupillary light reflex. Nursing staff failed to diagnose half of the cases (15/30) of anisocoria detected using the pupillometer device. Concordance between measurements for pupil size collected using the pupillometer, versus subjective assessment, was poor (Spearmen's rho = 0.75, IC: 0.70-0.79 P < 0.001). In 59 patients, 406 pupillary measurements were prospectively performed. The mean pupil light reactivity was 40 ± 7 %. 
We found only 3-pupil asymmetry (≥1 mm) in these volunteers (1.5 % of the population) with a clear pupil asymmetry during clinical inspection. In 200 healthy volunteers, intra-class correlation coefficient for maximum resting pupil size was 0.95 (IC: 0.93-0.97) and for minimum pupil size after light stimulation 0.87 (0.83–0.89). A blinded physician subsequently performed measurement using an automated pupillometer. 
Initially, nursing staff measured pupil size, anisocoria and pupillary light reflex. Patients admitted to these units after an acute brain injury were included. During another period, we conducted a prospective, observational, double-blinded study in two neurocritical care units. In order to determine inter-observer agreement of the device, we performed repetitive measurements in 200 healthy volunteers ranging in age from 21 to 58 years, providing a total of 400 paired (alternative right eye, left eye) measurements under a wide variety of ambient light condition with NeuroLight Algiscan pupillometer. To assess whether adoption of these technologies would benefit the clinic, we compared automated quantitative pupillometry with the standard clinical pupillary examination currently used for brain-injured patients. Several quantitative pupillometer devices are now available, although their use is primarily restricted to the research setting. The result seems to be a subjective measurement, with low precision and reproducibility. Current practice is to use a penlight to observe the pupillary light reflex. In critical care units, pupil examination is an important clinical parameter for patient monitoring.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
